Hospital revenue cycle management inefficiencies cost providers millions each year in lost income, and this is a single provider (and on average) estimate. When you examine hospitals collectively, this figure leaps into the billions.
In 2016, for example, hospitals lost an estimated 38 billion in uncompensated care revenue, and underpayment by Medicare and Medicaid almost tripled this staggering figure, according to the American Hospital Association.
Further, Medicaid expansion widened the uncompensated care fissure between providers in expansion and nonexpansion states.
To offset these losses, hospitals are creating their own revenue cycle management systems or contracting with revenue cycle management experts, and this rising trend is already changing the conversation. According to a recent Black Book survey, in fact, 80 percent of providers are considering outsourcing their hospital revenue cycle management in 2019.
Understanding Hospital Revenue Cycle
The simple definition of hospital revenue cycle management is the steps you must follow to ensure reimbursement for services rendered.
Revenue Cycle Management includes everything from software choice to pre-approving a patient via health insurance, from moving that patient through various revenue cycle steps until the services have been paid-in-full. This is a more complex and apt description.
It may sound simple, but understanding the hospital revenue cycle means being vigilant through the revenue cycle steps. Missing revenue cycle steps across multiple patients can cost your hospital millions. Effective revenue cycle management from beginning to end, unfortunately, means a tedious, sometimes lengthy, and meticulous set of procedures. “Computerized automation” is an increasingly important component for effective and efficient revenue cycle management designed to create a sustainable compensation and revenue stream.
Revenue Cycle Steps Simplified
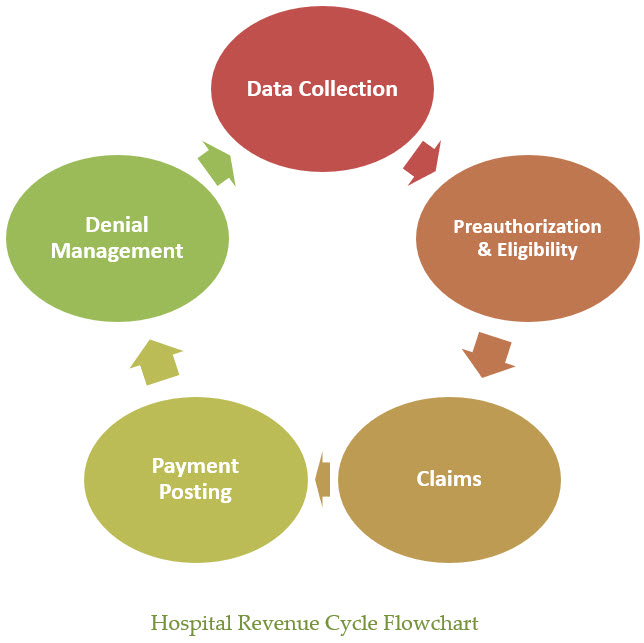
- DATA COLLECTION is the first of your revenue cycle steps.
- At this stage, a prospective patient has made an appointment.
- Staff must gather that prospective patient’s vital information and start a file.
- At this early stage, you are also deciding how to process patients, and making the right choices in technological applications and processing methods is crucial to the revenue cycle steps that come later.
- Inclusive software can handle your revenue cycle from beginning to end, but it is reliant on knowledgeable IT support and low-to-zero human error guarantees. These guarantees must remain across multiple patient charts and through several revenue cycle steps.
- PREAUTHORIZATION AND ELIGIBILITY are precursors to medical billing, and the revenue cycle management process in medical billing is perhaps the most important step when it comes to making sure your hospital is reimbursed for services rendered.
- At this stage, you have already collected the data from the prospective patient.
- Now you are verifying information with their insurance provider and learning the limits of coverage, including co-payments.
- With this step, you are getting your hospital preapproved to provide a service, equipment, medication, or other to this prospective patient.
- A preapproval letter for a unique procedure is sometimes provided by a patient’s insurer. Preapproval letters should be double-checked at the time of service because insurance coverage can change days after your hospital receives this letter.
- Because preauthorization and eligibility are precursors to billing, it is important to verify information methodically.
- The revenue cycle management process in medical billing must be as error-free as possible.
- CLAIMS submission is wide open to human error.
- When claims are submitted improperly, hospital revenue cycle management breaks down across the board, voiding the revenue cycle steps you have already taken and bringing the entire process to an impasse.
- Improper ICD-10 coding, for example, can find your hospital unpaid for services. Here you will want to analyze the details, look for typos and adhere to a meticulous charge capture structure.
- The revenue cycle management process in medical billing must be standard, repetitive and effective, but staff should be knowledgeable enough to adjust daily practices as needed.
- For example, is there a patient repayment schedule in place? Is all money due on the day of service? Is there a late fee implemented after a certain date? Are these rules waived or readjusted by circumstance?
- PAYMENT POSTING from insurers arrives after claims are accepted, but collecting patient portions of a bill can be time-consuming.
- Automated bills and reminders are a great option at this stage.
- Being vigilant at this step not only improves your revenue cycle, but it can also shorten your revenue cycle, bringing profits more quickly.
- DENIAL MANAGEMENT means taking a close look at denial statistics for your hospital, finding patterns in these denials, and putting the right changes in place to reverse that rate going forward.
- GENERATE REPORTS OFTEN to get a better idea of the revenue cycle steps your team is missing. Understanding hospital revenue cycle, after all, is mandatory when it comes to satisfying all the steps in revenue cycle management in healthcare.
Ask yourself a few questions before deciding the best way to manage your hospital’s revenue cycle. Are your team members experts when it comes to using inclusive software? Is your staff well-versed when it comes to understanding the hospital revenue cycle? Based on reports, are errors exceptionally low? What about the risk of future errors? Is your IT team helping to reduce error risks through perceptive tech utilization?
The steps in revenue cycle management in healthcare are many, but adhering to these steps is the best way to increase profits.
Best Practices for Profitability
A healthcare revenue cycle flowchart is a good way to think about the revenue cycle steps. Like any flowchart, the physical steps taken to increase profits should be performed in order. It is a repetitive process, but it does pay off.
Hospitals looking into how to improve hospital revenue cycle often come to the same conclusion, poor tracking of key performance indicators (KPI), and a segmented approach to the entire revenue cycle causes gaps.
In other words, even the smallest misstep can find your hospital uncompensated for services. Without KPI reports, it is difficult to know where breaks in the cycle are taking place.
A few tips on how to improve hospital revenue cycle include: (1) utilize technology such as patient portals to make collecting copayments easier, (2) utilize software that can verify coverage and eligibility electronically, (3) run reports often to see where missteps might be taking place in the revenue cycle process, (4) make sure patients are aware upfront of their payment portions, because patients disputing costs later can negatively affect your revenue cycle, and (5) educate relevant team members about each step in the revenue cycle, even if some of these steps fall outside their basic job description. A front-end team member, for example, might miss something in the data collection process and believe that it is not going to negatively influence billing. The team member may feel this way because the step was missed on another occasion and not addressed.
Revenue cycle management from beginning to end is a complicated endeavor, and the revenue cycle management process in medical billing is the hub when it comes to profits. It is also the foundation of every provider’s revenue cycle.
Success is ultimately measured through patient care and hospital profits.